Why do we have different blood types?
Blood type refers to the way blood is classified, usually referring to the type of red blood cells. Our blood type can be completely different from that of our friends or even family members. Knowing your blood type is very important, especially for blood transfusion and medical purposes. This begs the question: why do people have different blood types?
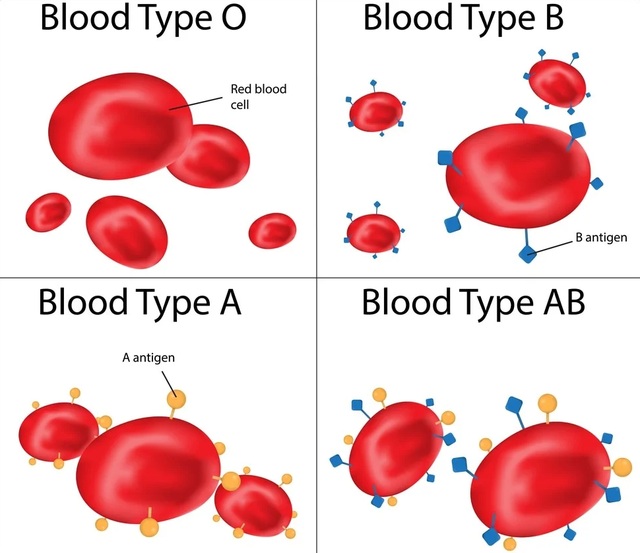
There are four main blood types in humans: A, B, AB, and O. Each blood type is determined by the genetic antigens present on the surface of red blood cells. Blood group A has type A antigens on red blood cells, blood group B has type B antigens, blood group AB has both A and B antigens, and blood group O does not.
Usually several antigens come from alleles of the same gene or are coding products of several closely linked genes, and these antigens form a blood group system. For humans, we have 30 different blood group systems that have been defined and recognized by the International Society of Blood Transfusion.
There are studies that suggest that the reason we have different blood types is malaria, and if you overlap the map of the malaria parasite with the map of blood type O, you will find that there is a difference between them. certain points of relevance.
Human blood is divided into several groups based on specific carbohydrates and proteins on red blood cells. For reasons that are not completely understood, the blood of each group may have antibodies against the other. Therefore, when transfused with blood from a different group, the recipient’s antibodies can destroy the transfused blood, causing harm to the body.
Malaria causes a large number of deaths every year. In 2020, an estimated 627,000 people will die from malaria globally. In people with the malaria parasite, infected red blood cells can build up in small blood vessels, preventing blood and oxygen from reaching the brain.
However, for people with blood type O, they are significantly resistant to malaria. A 2007 study found that people with blood type O were 66% less likely to develop severe malaria than people with other blood types.
This occurs when the parasite invades red blood cells, which express a family of repeated intercalated proteins (RIFINs) on its surface. According to a 2015 study, RIFIN acts like glue, allowing uninfected red blood cells to accumulate around infected red blood cells. At the same time, RIFIN binds strongly to the surface of type A erythrocytes but weakly to type O erythrocytes.
A blood sample can have more than 30 substances on the surface of red blood cells, and an individual’s blood type is one of several combinations of blood group antigens. Among more than 30 blood types, more than 600 different blood group antigens have been discovered, but most of them are rare or mainly found in certain ethnic groups.
However, blood type is not the only factor that affects a person’s risk of malaria, in addition to the antigens that make up the 4 main blood groups, there are 15 other antigens that can appear on the surface. red blood cells, which contain a class of antigens called the Duffy antigen.
People who lack the Duffy antigen will have a relatively strong resistance to one of the two main malaria parasites. And in fact, Duffy antigen deficiency is relatively common in sub-Saharan Africa, where the malaria problem is most severe, but rare in other parts of the world.
Scientists have found substantial evidence to explain why people in malaria-prone areas have blood type O. However, we still don’t know why blood types A, B and AB are relative. high elsewhere.
Some scientists have shown that there may be a disease link between different blood types. For example, people with blood type O are susceptible to cholera, plague, tuberculosis, and mumps. People with different blood types are more susceptible to other diseases; for example, people with blood type AB are more susceptible to smallpox, salmonella, and E. coli.
However, studies have yet to prove a cause-and-effect link between blood type and the incidence of these diseases, as other factors may contribute to the link. So these studies really found no evidence that blood type is protective or susceptible to disease, and malaria is the only disease that is actually related to blood type.
Currently, scientists don’t know why most people’s blood cells have a protein called rhesus factor (Rh factor) on their surface, which makes them Rh positive. About 15% of whites, 8% of blacks, and 1% of Asians lack this protein, and their blood type is Rh negative (often denoted by and – after the blood type, such as A or B-) .
Matching the Rh factor in the blood group is very important because a mismatch in the blood transfusion process (transfusion of Rh blood to someone with Rh- blood type) can lead to dangerous complications. However, people with Rh blood type have no problem receiving Rh- blood.
at Blogtuan.info – Source: cafebiz.vn – Read the original article here



